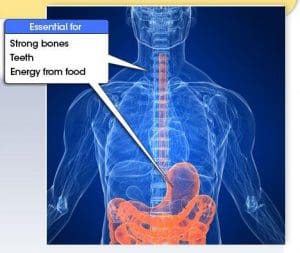
Phosphorus is a mineral found in bones and teeth. It is also involved in cell maintenance and helps in the production and storage of energy in the body.
When kidneys are working, they filter excess phosphorus from the blood through the urine to keep the right amount in the blood.
Normal Phosphorus levels in the blood are 2.5-4.5mg/dL and for anyone receiving dialysis, the phosphorus goal is 3.5-5.5mg/dL.
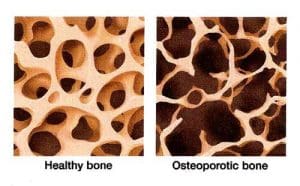 Why is it important to keep Phosphorus levels in range?
Why is it important to keep Phosphorus levels in range?
Higher levels that are out of range will send signals in the body to balance calcium and phosphorus in the blood so calcium is then pulled from the bones. Over time this activity will make bones weaker and more prone to fractures and breaks.
Where does the calcium go?
The calcium that has been pulled out of the bones is then circulating in the blood with nowhere to go so it starts to deposit in soft tissue including bone joints, skin, arteries, etc. Calcium deposits can cause pain and stiffening in soft tissues where it doesn’t belong and makes blood flow in those areas difficult.
Recommended dietary intake is 800-1000mg of Phosphorus per day.
Meats and dairy sources tend to be higher in phosphorus. The type of phosphorus in your food is important to know because of how much can be absorbed when digested.
There are two types of phosphorus organic and inorganic.
Organic Phosphorus is found in foods naturally (farm to table) that go through little to no processing. These foods contain phosphorus without chemicals. The absorption of phosphorus from plant-based foods and seeds is low, usually less than 50%, while up to 60% of phosphorus found in animal foods may be absorbed.
These foods contain phosphorus naturally:
- Fresh fruits
- Nuts
- Seeds
- Legumes
- Fresh vegetables
- Minimally processed grains
- Meats from the butcher
- Dairy
Leaching Phosphorus Through Cooking
Place meats/chicken/turkey/pork/seafood, etc. in a pot, cover with water and bring to a boil. Pour out the water and then use other cooking or preparation methods as usual to finish the cooking process including baking, grilling, sautéing, stir-frying, etc. It is best to avoid breading these meats using flour, egg and bread crumbs because they will add phosphorus to the finished product.
Inorganic phosphorus or phosphate is added in processing to many commercially prepared foods such as hot dogs, bacon, sausage, deli meats or cold cuts, processed cheese, prepackaged ready to eat convenience foods and snacks, frozen meals, bottled or canned beverages and baked goods. More than 90% of inorganic phosphorus can be absorbed by the body.
Phosphorus additives are used in adding color, improving flavor and increasing the shelf life of processed foods.
Phosphorus additives (chemical phosphorus) in foods can be found in the ingredients list on a food label:
- Dicalcium phosphate
- Disodium phosphate
- Monosodium phosphate
- Phosphoric acid
- Sodium hexameta-phosphate
- Trisodium phosphate
- Sodium tripolyphosphate
- Tetrasodium pyrophosphate
Added phosphorus in prepared foods adds to the amount that kidneys need to filter out to maintain a balance in the blood. When kidneys aren’t working well, less phosphorus is removed from the blood so the levels are then out of balance. Over time higher phosphorus levels will cause damage to the body such as seizures, bone disease, and secondary hyperparathyroidism.
There are medications that may be prescribed to help bind some of the phosphorus in a meal. Known as phosphorus binders, these medications are most effective when taken with a meal. The medication works like a magnet or a sponge attracting extra phosphorus in the stomach and intestines before it is absorbed into the bloodstream. The extra phosphorus bound by the medication is then eliminated out of the body though the colon with a bowel movement. If taken on an empty stomach, some discomfort or upset stomach may occur. As with many other medications it is recommended to take as prescribed.
The main goals for someone receiving dialysis is to stay healthy, feel good and have a good quality of life. The best way to do this is to follow the renal diet for the dialysis modality, either hemodialysis or peritoneal dialysis, take prescribed medications consistently, go to every scheduled dialysis session, stay the full treatment time and continue to see a primary care physician and any other healthcare providers as scheduled.
If kidney transplant is the main goal then the best candidates do all of the above and go to their scheduled transplant team appointments as well.
Professionals such as Dietitians are part of the healthcare team and are specially trained to help patients follow the renal diet. The renal diet can be combined with other diets for preexisting conditions such as diabetes or heart disease and can be adjusted for other dietary needs. Speak with your Dietitian or ask your physician for a referral to a Dietitian to start making dietary changes that will allow you to meet your healthcare goals.
Credit: Marisol Kramer, RD., Pure Life Renal of Stoughton
Educational materials can be found through these accredited sources:
National Kidney Foundation:
https://www.kidney.org/atoz/atozTopic_Brochures
https://www.kidney.org/atoz/content/dietary_hemodialysis
American Kidney Fund:
https://kitchen.kidneyfund.org/
Dialysis Patient Citizens:
https://www.dpcedcenter.org/staying-healthy/nutrition/nutritional-guidelines/
References:
https://www.kidney.org/atoz/content/phosphorus
Organic Phosphorus Versus Inorganic Phosphorus: Empowering Adult Kidney Patients With Nutrition Education Michelle Bump, MS, RD, CSR, LD Journal of Renal Nutrition, Vol 26, No 5 (September), 2016: pp e31-e33
Photo Sources:
http://drwolgin.com/osteoporosis/
http://www.nutrientsreview.com/minerals/phosphorus-phosphate.html